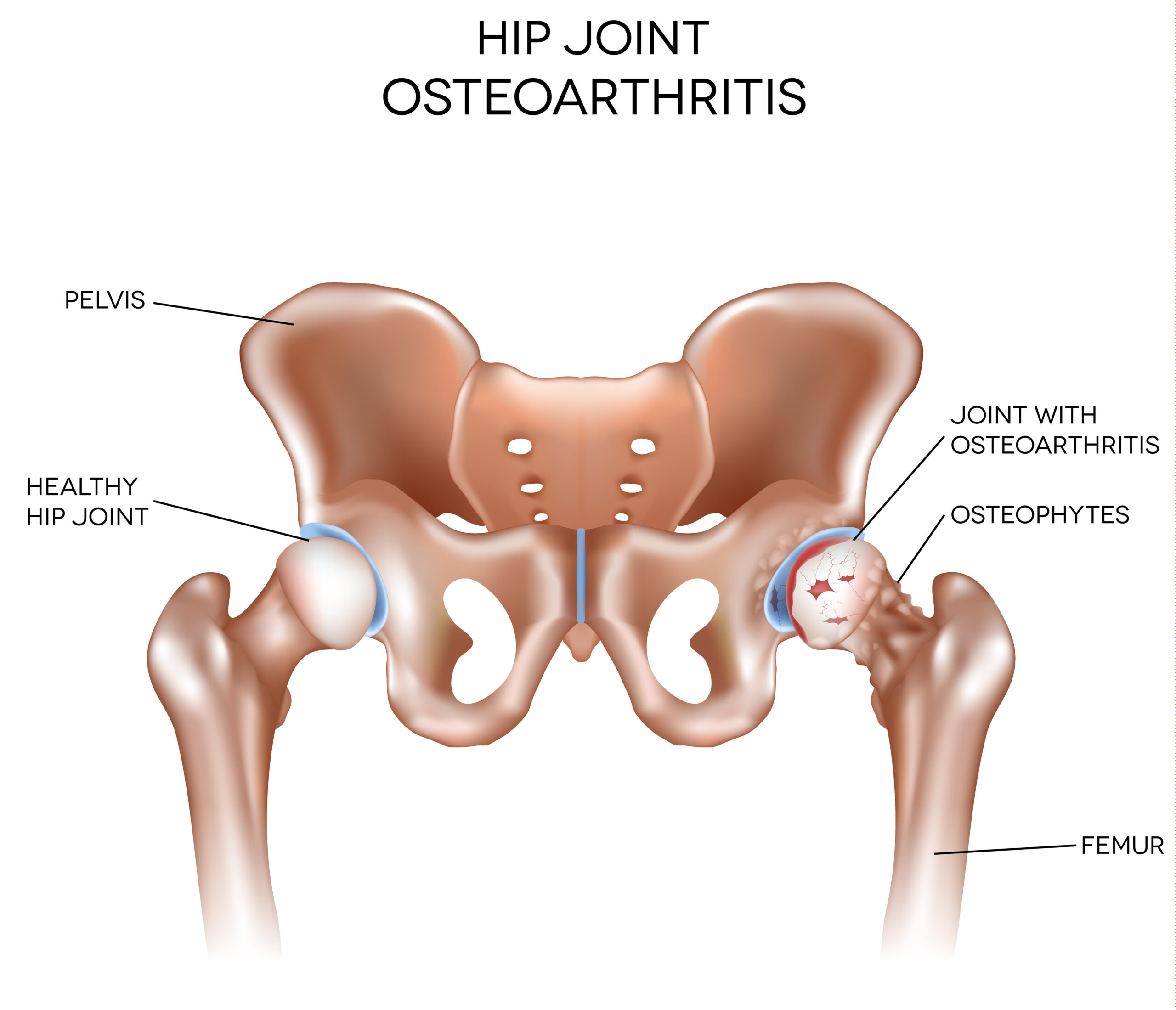
Hip Osteoarthritis
Osteoarthritis is a common degenerative joint condition that affects millions of people worldwide. Among the areas commonly afflicted by this condition, the hip joint is often a primary site of concern. Hip osteoarthritis can be debilitating, causing pain and reduced mobility. Hip osteoarthritis primarily results from the gradual deterioration of the cartilage that covers the hip joint’s bone surfaces. Over time, this protective cartilage breaks down, leading to bone-on-bone friction, inflammation, and pain.
Symptoms
1. Hip Pain: The hallmark of hip osteoarthritis is persistent hip pain, usually located in the groin region, which can radiate to the buttocks or thigh.
2. Stiffness: Reduced range of motion and stiffness in the hip joint, especially after periods of inactivity, are common.
3. Functional Limitations: Difficulty with daily activities such as walking, standing, and climbing stairs can be a significant challenge.
Risk Factors
Several factors increase the risk of developing hip osteoarthritis:
– Age: The risk rises with age, especially after 50.
– Genetics: Family history can play a role.
– Obesity: Excess weight places extra stress on the hip joint.
– Joint Injuries: Past injuries to the hip can contribute.
– Structural Abnormalities: Hip joint abnormalities can make it more prone to arthritis.
Diagnosis
Diagnosing hip osteoarthritis typically involves a combination of:
– Physical Examination: The healthcare provider assesses the patient’s symptoms and mobility.
– Medical History: Information about pain, stiffness, and functional limitations is collected.
– Imaging: X-rays or MRIs are used to visualize the hip joint and assess cartilage loss and joint damage.
Stages of Hip Osteoarthritis
Hip osteoarthritis often progresses through different stages:
1. Early Stage: Mild cartilage damage with minimal pain. Treatment primarily involves lifestyle modifications and pain management. Outcomes at this stage are generally positive, with symptoms often manageable.
 2. Moderate Stage: Cartilage loss is more significant, leading to moderate pain and stiffness. Physical therapy and medication become more essential. Steroid, gel, PRP injections stem cell injections may be utilized. Outcomes are favorable when these treatments are applied early and consistently.
2. Moderate Stage: Cartilage loss is more significant, leading to moderate pain and stiffness. Physical therapy and medication become more essential. Steroid, gel, PRP injections stem cell injections may be utilized. Outcomes are favorable when these treatments are applied early and consistently.
3. Severe Stage: Extensive cartilage loss results in severe pain and significant functional limitations. In some cases, hip replacement surgery (total hip arthroplasty) may be recommended. Alternative options include radiofrequency ablation of articular branches, which could provide 1-2 years of relief in pain. Outcomes post-joint-replacement-surgery are good, providing long-lasting pain relief and improved mobility. Post-surgery rehabilitation is crucial for optimal results.
Future Directions
As research in the field of osteoarthritis advances, we can anticipate more innovative treatments and interventions. These may include regenerative therapies, such as stem cell treatments, and improved prosthetic materials for hip replacements. Additionally, early detection and personalized treatment plans are expected to become more accessible, enhancing the management of hip osteoarthritis.
In conclusion, hip osteoarthritis is a prevalent condition with a range of causes, symptoms, and risk factors. Timely diagnosis and appropriate treatment are key to improving outcomes. With the promise of ongoing research and advancements, the future looks brighter for those living with hip osteoarthritis, offering hope for improved treatments and quality of life.